Clinical practice dilemmas: Managing respiratory illnesses on medical missions
December 6, 2018 |
Colds, pneumonia, sinus infections, and asthma are among the most common respiratory illnesses seen by medical volunteers working in developing countries. But with no X-rays or laboratory tests readily available, how do we decide if a child or adult has a simple viral infection, rather than one that might need antibiotics? Furthermore, how do we decide who is too sick to stay in their community for treatment?

Many short-term medical missions have clinical protocols for doctors who are accustomed to a North American style of clinical practice. How good are these protocols? Are these suggestions similar to international guidelines coming from bodies like the World Health Organization?
Our clinical protocols series continues with our recently published article in the Journal of Global Health Reports. In it, we analysed clinical protocols collected by contacting 225 organizations operating short term medical missions in Latin America and the Caribbean.
Most of the NGOs that responded had no protocols at all. Others had literature that they routinely recommended to volunteers. Fortunately, twenty organizations were willing to share their protocols for analysis.
You can find summaries of the most common recommendations for the treatment of upper respiratory illnesses, pneumonia, and asthma in the full article.
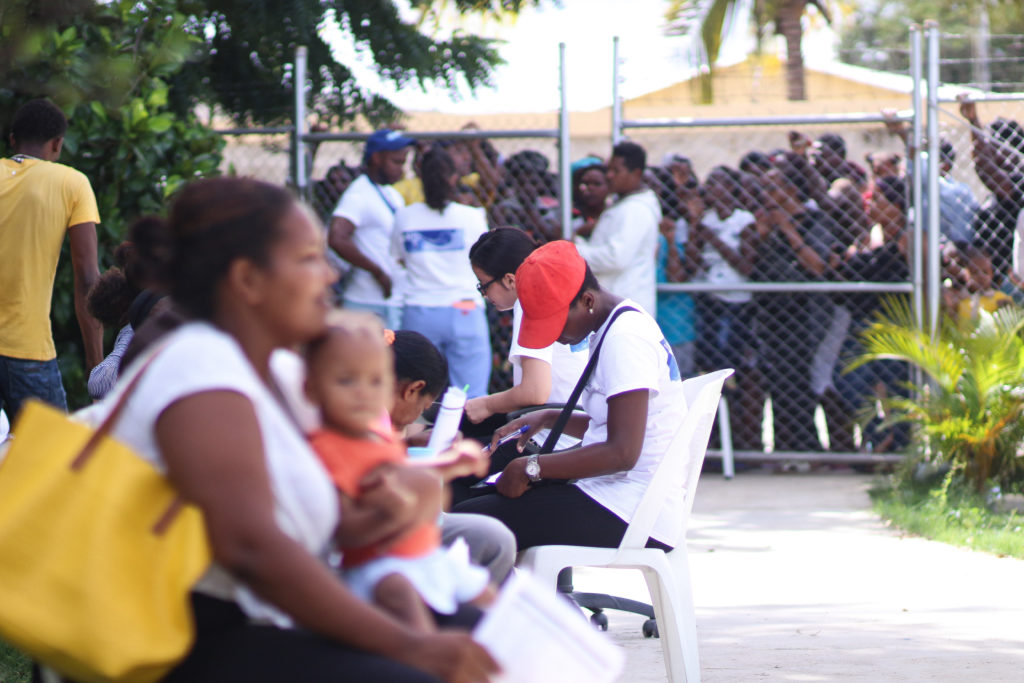
How do these protocols for respiratory illnesses compare to international guidelines?
On one hand, World Health Organization and other large bodies publish guidelines that generally reflect the best evidence available. They’re lengthy and broad. But as we’ve said before, locally developed protocols may better reflect local realities, including medication availability and resources. Good antibiotic stewardship should be more than a “gut feeling” on the part of the doctor.
Of course, this depends on how they were developed. For example, such clinical protocols can only work when locals participate in their creation. The care provided by volunteers should never compete with that provided by host clinicians. Furthermore, we identified many gaps in the protocols we analysed, meaning that there is still plenty of room for quality improvement on short-term medical missions.
Learn more about clinical guidelines for medical missions
Preparation and predeparture training by medical mission volunteers is a hot topic for medical mission research, but international guidelines for care in low resource settings are hard to find and access. So, we pulled out the most common evidence based recommendations, condensed them to make them bite-sized, and put them all in one place.
Read the published article on protocols for respiratory illnesses here. For more information on our guidelines initiative, check out our list of guidelines here. We’ve also previously published reviews of clinical protocols for gastrointestinal illness, diabetes and hypertension, and dermatologic disease.
We’ve also previously published reviews of clinical protocols for gastrointestinal illness, diabetes and hypertension, and dermatologic disease.
Register
Sign up for free to flag trips of interest and email organizations directly through our directory.
Comments
0 comments