Best practices: Eight things your medical volunteer mission might not do (but it probably should)
August 21, 2016 |

How should a medical volunteer mission make sure that it provides high quality care?
What clinical best practices should volunteers look for in a medical volunteer mission before they agree to donate their time and money toward a project in a developing country?
Below, we continue our summary of stolen gems from Greg Seager’s “When Healthcare Hurts”. Most are adapted from World Health Organization (WHO) standards of practice.
We have edited Seager’s suggestions for length.

1. Adopting a “less is more” approach to medication
The medicine your team distributes might be sold, traded, or misused because of cultural misunderstandings and illiteracy. First of all, keep things simple. A good formulary consists of 12 to 24 medications, dispensed in child resistant containers (never Ziploc bags). Except with “one-time” medications (antiparasitics and vitamin A), a pharmacist should also oversee dispensing in a private consultation room. Finally, leave surplus medication with medical professionals.

2. Using clinical treatment pathways to discourage variations in care
For example, Integrated Management of Childhood Illness (IMCI) can guide triage and case management for children under 5, and helps practitioners (and parents) to identify danger signs. Other pearls:

3. Getting patients to healthcare efficiently
Keep in mind the three delays in getting patients to a healthcare provider:

4. Putting patient safety on paper
Most importantly, every medical volunteer mission should have written safety protocols, a patient safety officer, and even malpractice insurance.

5. Empowering the host community
Never subvert the authority of local providers, who are the best equipped to care for their own communities. Collaborate with them and with regional healthcare services and workers.
6. Facilitating community projects
Ensure the host community leads the effort. Some ideas might include:

7. Training providers and communities
Training in best practices such as the GHEC Global Health competencies, Integrated Management of Childhood Illness (IMCI), and palliative care (HIV, spiritual training) can be high yield learning goals for providers.
Moreover, training for community health workers and translators has a higher impact than teaching the general population. Focus on healthcare seeking behaviour, nutrition, diarrhea management, and malaria prevention.
8. Keeping medical records and measuring outcomes
The WHO Millennium Goals prioritize impacts on child mortality, maternal health, and communicable disease. Measuring outcomes is difficult, but the chosen metric should be direct, objective, and practical.
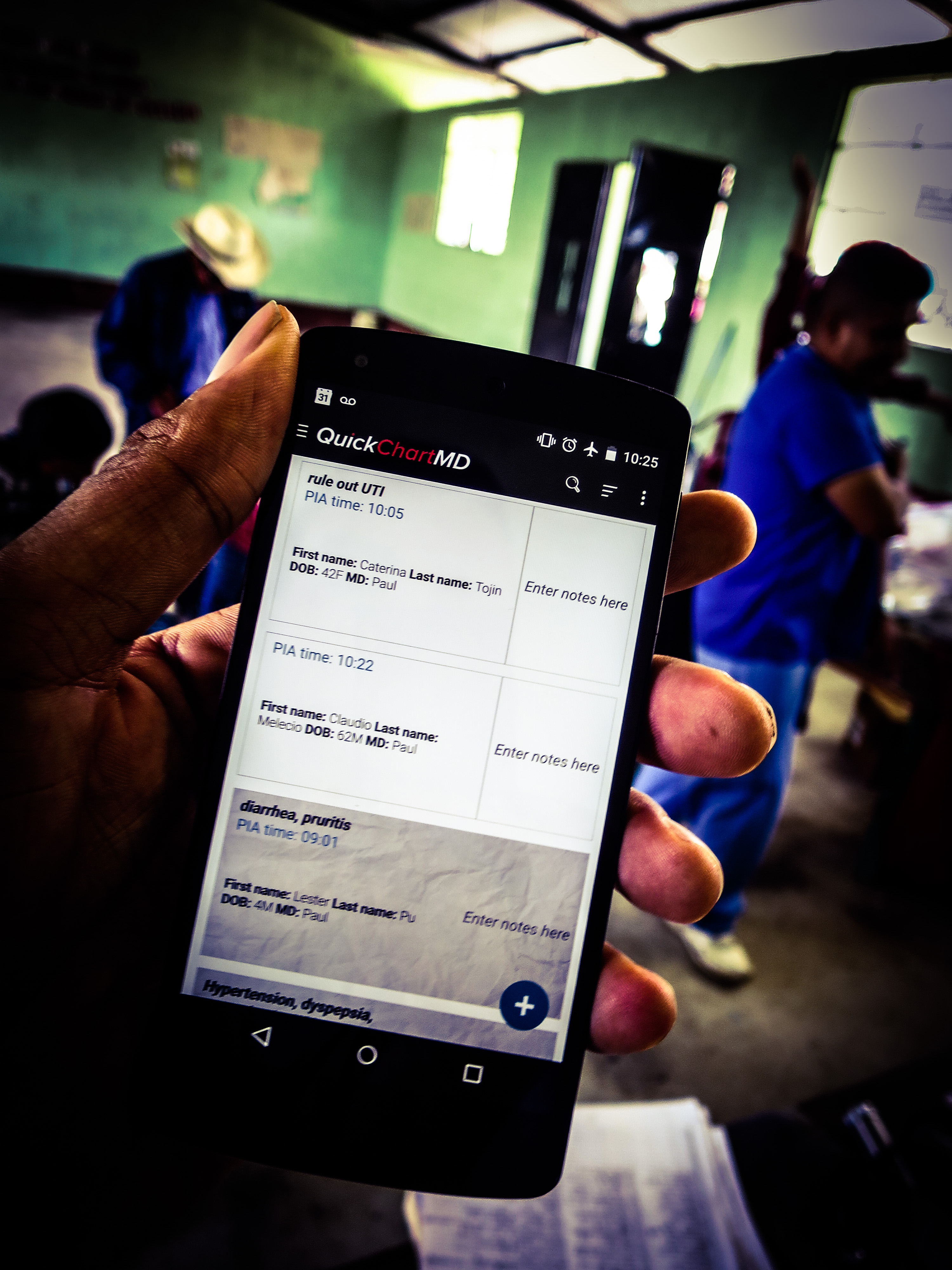
Furthermore, when the trip is over, send copies of patient medical records to local health services. One way to create such medical records is QuickChart EMR, our homegrown electronic medical records app designed for the remote settings in which medical volunteers often work.
Register
Sign up for free to flag trips of interest and email organizations directly through our directory.
Comments
0 comments